Community Health Needs Assessment
Evaluating the community’s health needs
For more than ten years, the six hospitals in Montgomery County have recognized opportunities to leverage community benefit resources, identify overlapping implementation strategies, and decrease duplication of efforts. In 2021, the hospitals further advanced their dedication to collective impact by developing a joint Montgomery County Hospital Collaborative (MCHC) Community Health Needs Assessment (CHNA) and Implementation Strategy.
The CHNA addresses 34 zip codes served by Adventist HealthCare, Holy Cross Health, MedStar Health, and Suburban Hospital, Johns Hopkins Medicine. The identified and prioritized health needs will guide the resources, program development, and collaborations required to address gaps in care, advance health equity, and improve quality of life. The MCHC CHNA used the information collected from primary and secondary data sources, including data from a community survey, to identify the top needs of the communities served. Once the needs were identified, local public health and hospital leaders, service providers and community advocates were engaged to set the priorities.
Three criteria were used to prioritize the needs identified from the primary and secondary data analysis: severity (high level of seriousness or urgency in the community), feasibility (could realistically improve in the next three years), and outcome (potential impact on the greatest number of people identified). Our stakeholders identified three priority areas and nine health factors, or root causes, as top unmet needs using the above criteria and their expertise and experience. The three priority areas are Access to Care; Healthy Behaviors; and Education, Income, Job & Environment. The nine health factors were then prioritized under each area. Each priority and health factor was ranked based on severity, feasibility and outcome.
The following is the ranked list of priority areas and associated health factors:
Access to Care
- Access to Mental Health Providers
- Access to Primary Care Providers
- Lack of Insurance
Healthy Behaviors
- Food Insecurity
- Adult Obesity
- Physical Inactivity
Education, Income, Job, & Enviornment
- Workforce/Labor Shortages
- Income Inequality
- Housing Cost Burden
Assessment Reports
FY 2022
FY 2020
- FY 2020 Holy Cross Hospital Community Health Needs Assessment
- FY 2020 Holy Cross Germantown Hospital Community Health Needs Assessment
FY 2017
In addition to identifying these nine root causes, the hospital collaborative also recognizes that racism is a key driver of disparities in mental and physical health outcomes. The graphic below demonstrates that systemic bias and structural racism cut across all social determinants of health and lead to inequities that have severe consequences. By addressing root causes and focusing on inequities due to racism, a reduction in the top health outcomes—heart disease, diabetes, mental health, cancer, maternal and child health, infections, and unintentional injuries—can be achieved.
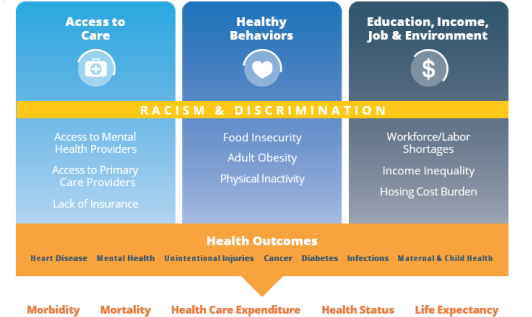
Holy Cross Health routinely conducts community health needs assessments to help us and our community partners plan programs. The assessment focuses on the geographic areas served by Holy Cross Hospital and Holy Cross Germantown Hospital.
Year-round, we gain insight into the county’s unmet health needs by being involved in community coalitions, commissions, committees, boards, partnerships, advisory groups and panels. We also gather information in collaboration with the Montgomery County Healthy Montgomery Community Health Improvement Process.
In addition, we examine other important data including:
- Population demographics
- Area socioeconomic factors
- Resident use of health services
In our FY 2020 needs assessment, Holy Cross Health identified the following target areas of need:
- Maternal & Infant Health
- Seniors
- Diabetes
- Cancers
- Cardiovascular Health
- Obesity
- Behavioral Health
Three overarching themes were also identified:
- Lack of access to care
- Health inequalities
- Unhealthy behaviors
Once an annual plan has been developed, additional input is gathered from a diverse group of people, including:
- Representatives from county and state health departments
- Individuals or organizations serving the medically underserved, low-income and minority population
- Individuals or organizations representing the broad interests of the community
Their recommendations for the system's community benefit initiatives are critical to the success of these initiatives.
